Intravitreal Injection for Macular Oedema
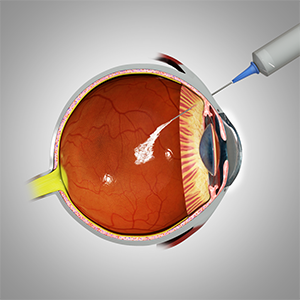
What is Intravitreal Injection for Macular Oedema?
An intravitreal injection is a non-invasive eye procedure where medication is injected into the vitreous cavity - the space at the back of your eyes, near the retina. The vitreous cavity is filled with vitreous humour gel, a jelly-like fluid.
What are the Indications for Intravitreal Injections?
Intravitreal injection is recommended for numerous retinal conditions. These include:
- Diabetic retinopathy: A condition where a person has an abnormal growth of blood vessels in the retina, commonly seen in diabetic patients
- Macular edema: Abnormal swelling in the macula, the part of your eye that provides sharp, central vision
- Age-related macular degeneration (AMD): An eye disorder marked by diminished central vision over time
- Retinal vein occlusion: A blockage in the veins that carry blood away from the retina and out of your eyes
- Infections such as endophthalmitis and uveitis marked by swelling and inflammation within your eye
Sometimes, an intravitreal injection is given as part of routine cataract surgery to administer medications such as antibiotics and steroids. This minimizes the use of drops post-surgery.
What are the Medications Given Through Intravitreal Injections?
Your ophthalmologist may administer medications such as:
- Intravitreal steroids
- Antibiotics
- Antiviral drugs
- Anti-fungals
These medications help reduce leakage of vitreous humour gel and also minimize infections caused due to germs.
Sometimes an intravitreal injection may be used to insert a tiny gas bubble into your eye to help in the repair of a retinal detachment.
Procedure: How is an Intravitreal Injection Administered?
The procedure is performed by a trained retina specialist at an ophthalmologist’s clinic or an eye hospital.
You will sit in a recliner chair for the procedure. Your ophthalmologist will anaesthetize your eye and eyelids using a numbing gel or drops to reduce pain from the intravitreal injection. After this, your eye and the eyelids may be cleaned using a sterile solution of povidone-iodine, a yellow coloured liquid, which is effective in killing the bacteria that live around your eyes. During this procedure, special eye equipment called an eyelid speculum may be used to keep your eyelids open.
Before injecting the intravitreal injection, your ophthalmologist will ask you to look in a specific direction to facilitate placement of the injection. Then, the injection will be administered using a tiny needle through the white part of your eye called the pars plana. You may feel some slight pressure with little or no pain during the injection. After the injection, the speculum will be removed and your eye is cleaned.
The entire procedure is completed within 30 minutes.
What to Expect after an Intravitreal Injection?
You may experience slight bleeding in the white part of your eye after an intravitreal injection. This is normal and will subside.
You may be prescribed artificial tears to provide relief from dryness and surface irritation. You should follow the instructions given by your ophthalmologist.
- Use eye drop medicine as directed.
- Avoid the following:
- Rubbing your eye
- Doing work in front of the computer screens for long hours
- Swimming for minimum of 3 days
What are the Risks and Complications of an Intravitreal Injection?
Though an intravitreal injection is relatively safe, it may have certain side effects that may include:
- Bleeding
- Inflammation
- Floaters
- Infection
- Retinal detachment
- Vision loss
Your ophthalmologist may check the pressure within your eye called intraocular pressure (IOP) after the injection as there could be a temporary rise in IOP. It usually returns to normal after some time. People with glaucoma may require more time to bring down the IOP and should be monitored.
When Should You Visit an Eye Specialist After an Intravitreal Injection?
You should visit an eye specialist if you experience any of the following symptoms after the procedure:
- Decreased vision
- Increased light sensitivity
- Eye pain or discomfort
- Increased floaters after the first day
Thereafter, you should visit as per your eye specialist’s recommendations.
Do you Require more than one Session of an Intravitreal Injection?
Some people may require repeated intravitreal injections for chronic conditions such as diabetic retinopathy, macular edema, AMD, and retinal vein occlusion. Intravitreal injections are usually safe and well-tolerated over several years. Your ophthalmologist will perform certain tests to ascertain whether you require further intravitreal injections or alternate treatment.
Related Topics:
- Lifestyle Lenses for Cataracts
- Toric Lenses
- Multifocal Lens Implant
- Refractive Lens Exchange
- Cataract Surgery in People with Retinal Diseases
- Age-Related Macular Degeneration
- Diabetic Retinopathy
- Retinal Vascular Diseases
- Anti VEGF
- Eylea (Aflibercept)
- Lucentis
- Avastin
- Intravitreal Steroids
- Ozurdex
- IIuvien
- Retinal Laser (Pattern and Micropulse/Subliminal laser)
- Oral Immunosuppression for Uveitis
- Treatment for Cataract
- Cataract Surgery in Diabetics
- YAG Capsulotomy
- YAG Iridotomy
- Macular Laser for Central Serous Retinopathy
- Macular Laser for Macular Oedema
- Cataract Surgery in Ocular inflammation
- Retinal Laser therapy
- Treatment of Posterior Uveitis
- Selective Laser Trabeculoplasty
- Treatment of Glaucoma
- Retinal Disease Treatment
- Intraocular Lens (IOL)
- Digital Retinal Photography
- Intravitreal Injection for Macular Oedema
- Treatments for Diabetic Macular Oedema
- Treatments for ARMD
- Ocular Ultrasound
- Gonioscopy
- Panretinal Photocoagulation
- Panretinal Photocoagulation for Ocular Ischemic Syndrome
- Treatment for Vein Occlusions
- Treatment of Acute/Chronic/Recurrent Iridocyclitis