Retinal Detachment
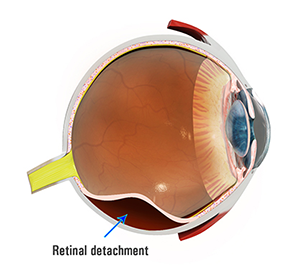
What is Retinal Detachment?
Retinal Detachment is an eye disorder in which the retina (light receptive layer of tissue at the back of the eye) is pulled away from its normal position. In retinal detachment, the retina gets separated from the underlying choroid (layer of blood vessels that supplies oxygen and nutrients to the retina) and leaves the retinal cells deprived of oxygen. Certain risk factors, such as ageing, severe near-sightedness, eye injury, cataract surgery, and family history, can increase the chances of retinal detachment. If not treated early, this condition can cause permanent vision loss.
Symptoms of Retinal Detachment
Certain symptoms appear as warning signs and almost always appear before retinal detachment can occur or become more severe. The characteristic signs and symptoms that indicate the onset of retinal detachment include:
- Sudden onset of blurred vision
- Partial vision loss (as if a grey curtain is moving across the field of vision)
- Eye floaters (tiny specks or strings floating in the field of vision)
- Eye flashes (the illusion of flashing lights in the side vision)
- Shadows or blind spots (areas of darkness) in the field of vision
Depending on the cause, three types of retinal detachment are observed:
Rhegmatogenous retinal detachment (RRD): This is the most common type of retinal detachment and is associated with a hole or tear in the retina. Fluid from the vitreous humour (jelly-like centre of the eye) seeps through the retinal hole and accumulates in the space between the retina and the underlying retinal pigment epithelium (RPE), thereby lifting the retina. RPE, located between the retina and the choroid layer, is a pigmented cell layer that nourishes the retinal cells.
Tractional retinal detachment (TRD): It is the second most common type of retinal detachment. TRD occurs due to the formation of scar tissue or growth of other abnormal tissue on the surface of the retina, separating the retina from the underlying RPE. TRD is commonly observed in people with uncontrolled diabetes, previous retinal surgery, or chronic inflammation.
Exudative retinal detachment: This type occurs when blood or fluid from the choroid leaks into the space between the retina and the underlying RPE, causing a detachment. This is an uncommon complication of conditions such as hypertension, eye tumours, and rare blood vessel disorders.
To diagnose retinal detachment, a comprehensive eye examination is performed; wherein the physical appearance of your eye, vision, eye pressure and your ability to see colours is tested. Your doctor instils eye drops to dilate your pupil in order to see your retina properly. An ultrasound may also be ordered in certain cases.
Treatment for Retinal Detachment
There are several methods to treat retinal detachment. These include:
- Scleral bulking
- Sutureless vitrectomy
- Tamponade
- Silicone oil
- C3F8/SF6
Related Topics:
- Uveitis and Ocular Inflammation
- Dry Eyes
- Lid Cysts
- Blepharitis
- Glaucoma
- Retinal Tear
- Cataract
- Diabetic Macular Oedema
- Retinal Vein Occlusion
- Macular Oedema
- Cystoid Macular Oedema
- Central Serous Retinopathy
- Vision Disorders
- Watery Eye
- Tear Duct Obstruction
- Vein Occlusion
- Chalazion
- Vein Occlusion Macular Oedema
- Allergic Disorders of the Eye
- Blurred Vision
- Distortion of Central Vision
- Ocular Ischemic Syndrome
- Optic Neuropathy
- Posterior Uveitis
- Proliferative Diabetic Retinopathy
- Temporal Arteritis
- WET AMD
- Traumatic Iritis
- Acute/ Chronic/Recurrent Iridocyclitis
- Am I at Risk of Glaucoma?
- Epiretinal Membrane
- Open and Closed Iridocorneal Angles
- Pars Planitis/Intermediate Uveitis
- Retinal Detachment
- Subconjunctival Haemorrhage